We know seaweed changes gut Microbiome. There are more than 10 times more bacteria in the gut (microbiome) than cells in human body!
Moreover, there are more than 150 time total genome of microbiota than the human body. Mounting evidence suggested that gut microbiota plays an important role in the development of disease in the brain. And there is a bidirectional relationship between the brain, gut, and the microbiota within the gut, which is referred as the microbiota-gut-brain axis.
Seaweed Changes Gut Microibiome in Animal Studies
In a 2017 study Dr Sunil Panchal and Prof Brown[1] put rats onto a obesity inducing diet. They had 3 groups of 10 rats each.
- Group 1 had normal rat diet.
- Group 2 had a Junk food diet.
- Group 3 had the Junk food diet plus some seaweed (Kappaphycus sp) and in human terms that was about 13 gm per day.
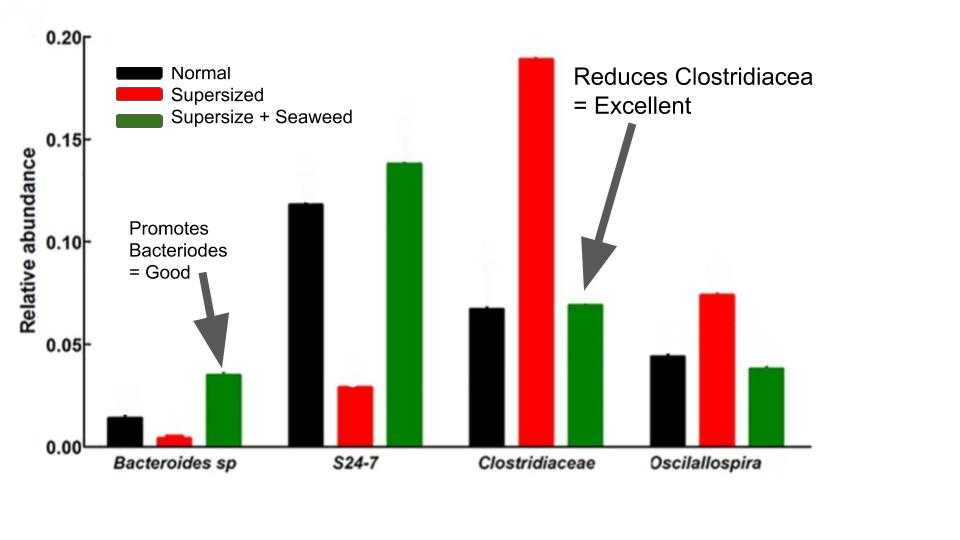
At the end of the 8 week trial they looked at the gut microbiota. Find the full details in the references, but this graph stands out.
There are 4 families of bacteria. The black lines is from the feces of the normal food rat. The Red lines are from those Supersize diet, and the Green is from the Supersize plus seaweed.
Bacteriodes species – 3 times more. This is a strong marker for obesity so it helps explain why the seaweed reversed obesity. Seaweed has over 30% sulfated polysaccharide (carrageenan) and it is a good food source to the bacteria A recent study has shown that Bacteroides sp. are able to digest carrageenan
producing oligosaccharides which possess lipid-lowering properties.
In the s24-7 type seaweed increased the counts back to above the normal.
In the Clostridiacea and the Osciallspira back to normal
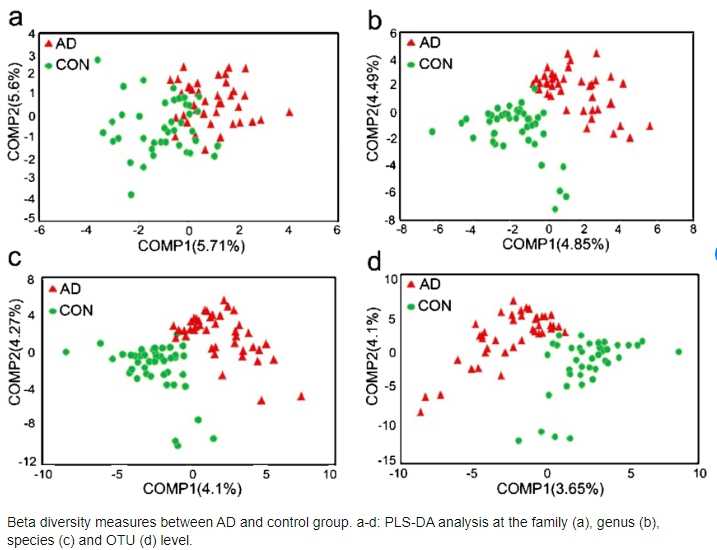
Microbiota in Alzheimer Disease
While improved microbiome helps in diseases such as blood pressure, obesity, there is also a growing body of evidence that microbiome is important in Alzheimer’s Disease.
Here is 1 figure between 40 patients with AD compared with “normal” patients. Read more in Dr Zhung’s paper.
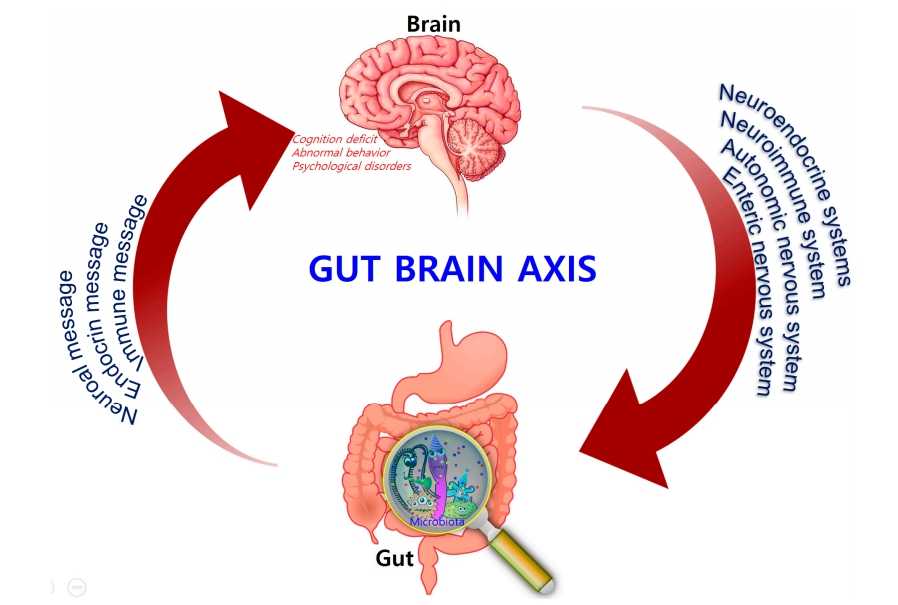
The Microbiota–Gut–Brain (MGB) Axis
The concept of the MGB axis is well established. The neuroendocrine and neuroimmune systems, in addition to the sympathetic and parasympathetic arms of the autonomic nervous system (ANS) and the ENS, are key pathways in gut–brain communication. Although the exact mechanisms mediating gut–brain interactions are not fully understood, they were suggested to involve endocrine, immune, and neural pathways (vagus nerve and enteric nervous system), leading to possible alteration in AD patients or aggravating inflammation.
The concept has now expanded and has become a quickly evolving area of research that led to convergence of research efforts in the fields of neuroscience, psychiatry, gastroenterology, and microbiology—disciplines that were previously considered to have distinct and separate research objectives and focuses.
Further, depending on the diet that the Microbiota is living on has a cascade effect on compounds made, adsorbed and therefore the makeup of that microbiota.
No longer. It is clearly integrated, and treating them as a whole system is now essential.
 [/vc_column_text][/vc_column][/vc_row][vc_row css_animation=”” row_type=”row” use_row_as_full_screen_section=”no” type=”full_width” angled_section=”no” text_align=”left” background_image_as_pattern=”without_pattern”][vc_column][vc_column_text]
[/vc_column_text][/vc_column][/vc_row][vc_row css_animation=”” row_type=”row” use_row_as_full_screen_section=”no” type=”full_width” angled_section=”no” text_align=”left” background_image_as_pattern=”without_pattern”][vc_column][vc_column_text]
REFERENCES
[1] Wanyonyi, S, du Preez S et al 2017 Kappaphycus alvarezii as a Food Supplement Prevents Diet-Induced Metabolic Syndrome in Rats. Nutrients 9 (11) DOI:10.3390/nu9111261 (Pubmed)
[2] Li, M.; Shang, Q.; Li, G.; Wang, X.; Yu, G. Degradation of marine algae-derived carbohydrates by Bacteroidetes isolated from human gut microbiota. Mar. Drugs 2017, 15, 92
[3] Dinan, T Cryan, J 2017 Gut instincts: microbiota as a key regulator of brain development, ageing and neurodegeneration Journal of Physiology 595 (2) 489-503 https://doi.org/10.1113/JP273106
[4] Zhuang ZQ, Shen LL et al. 2018 Gut Microbiome is Altered in Patients with Alzheimer’s Disease (2018) Journal of Alzheimer’s disease: JAD 63(4):1-10 · https://doi.org/10.3233/JAD-180176
[5] Vo Van Giau OrcID, Si Ying Wu 2017 Gut Microbiota and Their Neuroinflammatory Implications in Alzheimer’s Disease Nutrients 2018, 10(11), 1765; https://doi.org/10.3390/nu10111765